Loading
Loading

At Epiphany Dermatology, providing access to the best dermatologic care is our top priority.

Your Skin Cancer Specialists

At Your Service

Expert Patient Care
A Full Suite of Dermatological Services
Epiphany Dermatology is committed to offering the highest standard of dermatologic care. Our board-certified dermatologists, physician assistants, nurse practitioners, and aestheticians offer a wide range of dermatology services—from skin cancer care and acne treatments to general dermatology and cosmetic services.
We work collaboratively with our patients to personalize their treatments and help them look and feel their best.
Book an Appointment

Mohs Surgery (On-Site Skin Cancer Removal)
Mohs surgery spares the most amount of normal tissue and has the highest cure rates for many non-melanoma and melanoma skin cancers. It’s the gold standard of care in non-melanoma skin cancers and is commonly used in the treatment of some melanomas.
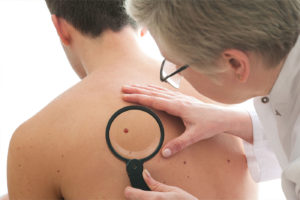
Biopsies
A biopsy is the removal of a piece of skin to help render a diagnosis of skin cancers or inflammatory conditions. Dermatologists biopsy an area to confirm a diagnosis that cannot be rendered with the eyes alone. We need a microscope to be certain.

Acne Treatment
Acne can have a big impact on your life, which is why we take acne treatment very seriously and use aggressive treatment plans when necessary. Our staff is passionate about treating acne to prevent the emotional and physical scars that can last a lifetime.

Chemical Peels
Most people don’t realize that there are several kinds of peels great for improving the appearance of the skin. Chemical peels should be done in a series of three to six peels. For best results, we recommend a series of six peels, three weeks apart.

Juvéderm®
If you’re looking for non-invasive ways to treat fine lines and wrinkles, chances are Juvéderm has been discussed. While classified as a filler, Juvéderm is a sweeping term for a collection of hyaluronic acid fillers with each product targeting a specific area of the face.

Fillers
Injectable fillers help restore volume in the skin, which can reduce the appearance of lines and wrinkles that come with age. Injectable fillers have also been used to make thin lips fuller, correct acne scars, and make the areas under the eyes less dark or puffy.
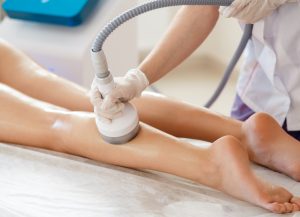
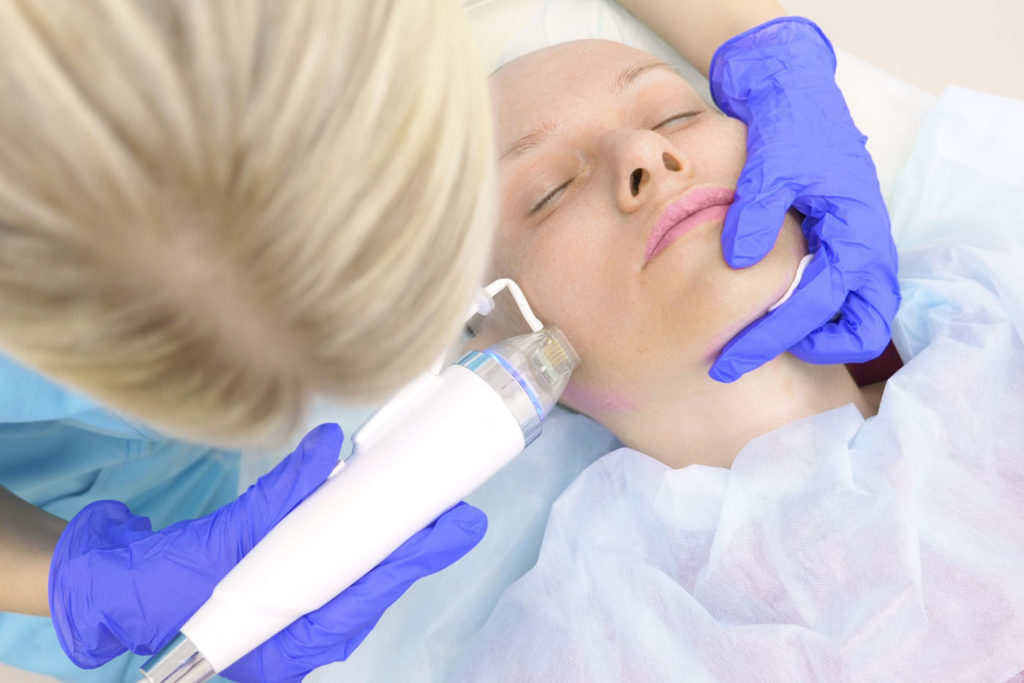
Body Contouring (CoolSculpting®, EMSculpt®, SculpSure®, etc)
Body contouring improves the contour of the body by heating, freezing, or applying energy to targeted areas. Using non-invasive devices, we can remove fat, tone muscle, and tighten the skin to enhance the overall body contour appearance.
We work hard to ensure everyone has access to affordable skin care.
We believe everyone should have prompt access to the best skin care, regardless of where they choose to live and raise their family. Gone are the days of waiting many months and driving countless miles to see a dermatologist.


Skin Care Products at Your Fingertips
Shop our full lineup of physician-approved skin care products. We’ve hand-selected each product in our store based on what our providers use in the office, offering you the same quality of skin care products we use ourselves and recommend to our patients.